Skin services
About the clinic
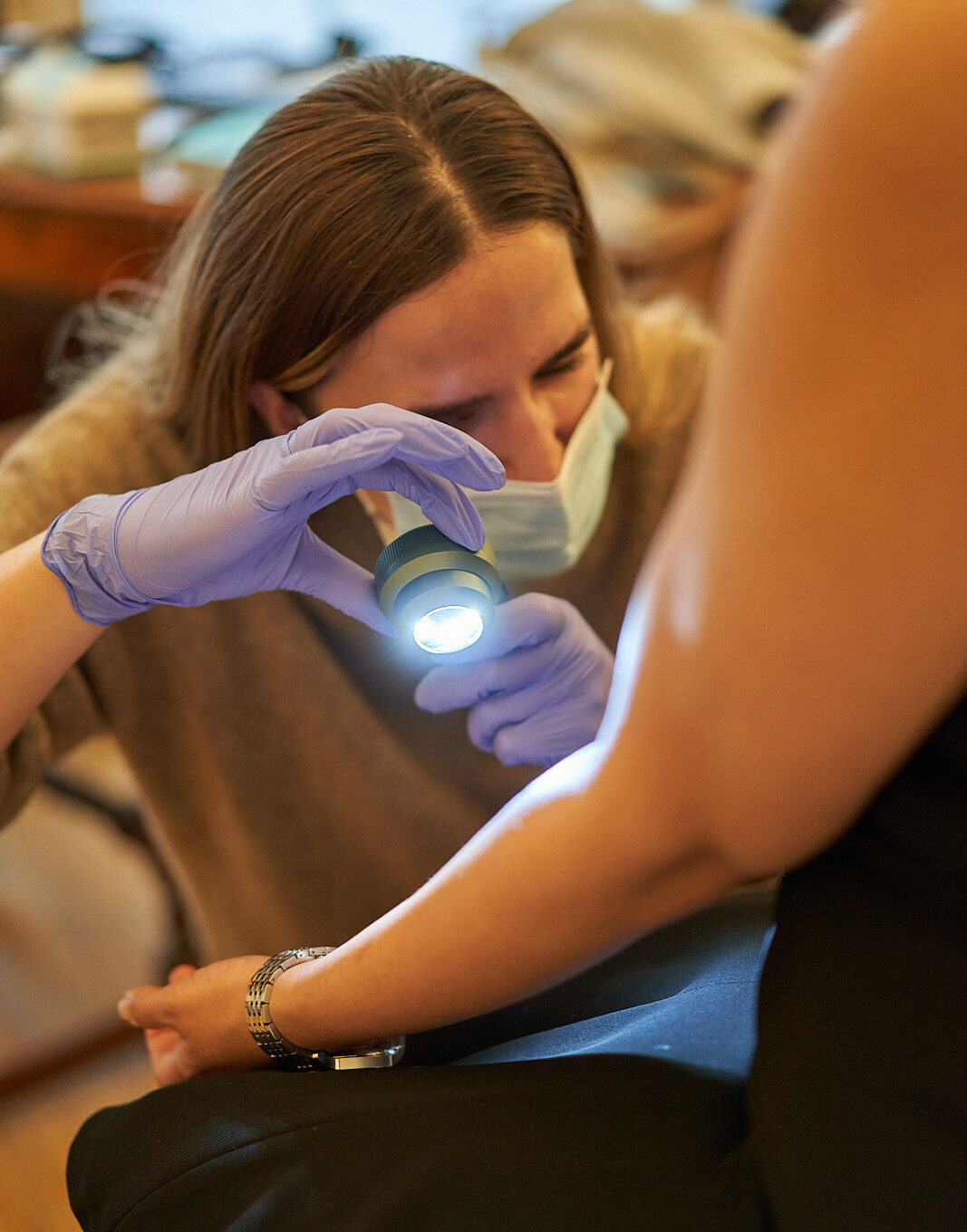
We provide a ‘one stop’ service, from consultation to minor operations, with same day procedures performed in our on-site Day Surgery without the formalities and administrative delays caused by hospital admission. Our experienced team can treat adults and minors over the age of 12.
Patient information
Book an appointment
You can call, email or complete a form to book your appointment. We are always happy to help.
Fees & Payment
Here you will find information about costs related to our services. This helps us be more transparent to you.